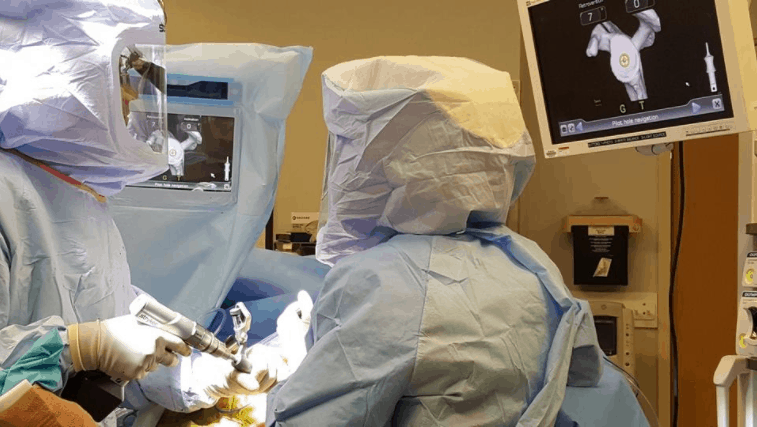
YORK, Maine – Dr. Mayo Noerdlinger looks up at a computer screen above his head during a shoulder replacement surgery one recent morning at York Hospital. A 3-D image of the patient’s shoulder system floats on the screen, an image that has been created preoperatively and allows him to decide in advance how he wants to proceed during surgery.
Soon, a GPS probe is placed in the patient’s bone, picking up the contours of her shoulder and matching that to the image taken before surgery. As Noerdlinger works to put the pins in the bone to hold the replacement piece in place, he is guided by the probe to place them precisely where they need to go, down to the millimeter. No chance they will be put in “cockeyed.”
Noerdlinger said the technology represents the next and important step in the evolution of shoulder operations. York Hospital is the first hospital in the Northeast to offer this kind of technologically-guided surgery, and has been offering them since June.
“I definitely think there’s value in having a doctor who has experience and who has done a lot of surgeries,” said Noerdlinger, an orthopedic surgeon with Atlantic Orthopaedics and Sports Medicine in Portsmouth. “But even a person who does a lot of them may have an off day. A lot of experienced surgeons look at this technology and say, ‘Yeah, yeah, you’re not going to get better than surgical experience.’ But I think that there’s a little hubris in that.”
Noerdlinger certainly qualifies as an experienced surgeon. He has been a practicing physician for 15 years, and in the Seacoast area is the go-to-guy for shoulders. He said shoulder surgery has seen advances over the years. Where once there were one-size-fits-all components, today components are size-specific for each patient. This “has indeed led to getting good to excellent results for 15 to 20 years. But can we do better?”
He said when he was shown the equipment created by the company ExactechGPS, which allows those pins to be placed accurately in the bone, he saw the next logical step in perfecting patient outcome. “I’ll be honest with you. I’m not sure that putting in the components perfectly will make a difference. But it makes common sense,” he said, that perfect placement of the pins could allow the replacement shoulder to last five to 10 years longer. “I think this is a game changer.”
Shoulder problems are typically caused when the cartilage that protects the shoulder bones has worn down due to years of motion and pressure. This causes arthritis, most typically osteoarthritis, but also rheumatoid arthritis. Patients also can be suffering from bursitis.
Not all people with shoulder issues are candidates for total replacement. Many issues can be repaired through arthroscopic surgery, Noerdlinger said. For instance, most people he sees have a rotator cuff tear that can be handled through a shoulder arthroscopy. Many patients choose cortisone or similar treatments that will stave off the pain for a period of time, rather than go through surgery at all.
He said he sees people in their 30s and 40s who have shoulder issues, but can deal with it through a variety of treatments including cortisone – and yoga. “Staying flexible is key,” he said. “But by the time they’re in their 50s and 60s, they’re tired of it. They say, ‘I don’t want to live with it and I’ve had all the cortisone injections I want to have.’”
The ExactechGPS system begins to work at his office, he said. Patients who decide on replacement will get a CAT scan, which the company turns into a 3-D image. With this image, Noerdlinger can come up with a game plan specifically geared for the individual patient. He said this is particularly helpful when preparing for a reverse shoulder replacement – when the ball at the end of the humerus bone is cut off and a metal ball is attached to the upper arm bone – essentially reversing the shoulder system. This is done when there is a large rotator cuff tear. Rather than the rotator cuff, the deltoid muscle will power the arm.
Armed with patient-specific information, he goes into surgery, where he places a probe into the shoulder blade that will allow him to place the ball component exactly in the right place and pin it into the bone precisely. And it’s all on the computer screen in front of him.
He said creating the hole for the probe, or tracker, “does add to surgical time, and that’s more anesthesia. But I’ve found the typical increase in surgical time is four minutes. That’s worth it to put those pins in perfect position. I started performing these at the end of June, and this is my ninth. There have been no negative outcomes. Everyone is doing well.”
Noerdlinger credits York Hospital President Jud Knox and the hospital Board of Trustees for listening to him when he approached them about acquiring the machine. “It’s an expense that the hospital took on themselves, and they do not pass on to the patient,” he said. “Our practice has a great relationship with the hospital, and they always said, if you want something let us know. This was the first time I went to the hospital, and they listened to me.”
Noerdlinger said he is waiting for Portsmouth Hospital, where he is Chief of Orthopedic Surgery, to get the same machine, but because the hospital is part of a larger, for-profit corporation, “there’s a lot of machinations. York Hospital made a decision in a week. This hospital said, ‘Why not do it?’”
This is not the first high-tech machine that the hospital has acquired. Since early 2016, the hospital has offered knee replacement surgery using a similar technological system that marries preoperative images with operation images. In both cases, York Hospital was the first in the region to offer these technologies.
Knox said much of the hospital’s decision-making comes down to the relationship with the doctor and the outcome for the patient.
“I don’t think being the first in the region is a risk for us if, one, we have a great relationship with the physician who’s promoting the technology and, two, if the evidence is available to show the efficacy of the technique,” he said. “And whatever we’re talking about, we try to figure out if it has value for patients.”
Unlike knee replacement surgery – estimated by the American Academy of Orthopaedic Surgeons at some 900,000 a year nationwide – only about 56,000 shoulder replacement surgeries are performed annually. “It’s a non-weight-bearing joint, unlike knees and hips,” said Noerdlinger. “The question is, how much money should be spent to make someone’s life better? That analysis is above my pay grade. I believe this will allow people to have a better long-term outcome. I can’t monetize that value. But I do feel passionate about this.”
“When you look at the disability caused by shoulder problems, it’s huge. When people can’t put on their shirt or tie their shoes, that’s an issue,” said Knox. “We won’t do as many shoulders as knees, but the numbers don’t mean those shoulder operations are not important. There is not a single number of frequency that we use to measure whether we do a procedure or not.”
According to Noerdlinger, York Hospital is among a rarified few that have embraced this technology. There are only five major medical centers that have this machine in operation or are in the process of setting it up, including Stanford University Medical Center, the Cleveland Clinic and the Hospital of Joint Disease at New York University. It is also widely used in Spain, France, England and Australia. Few small hospitals are using the technology.
“The significance is York Hospital’s relationships with patients and their physicians,” said Knox. “Hopefully that’s our strength and hopefully that’s what helps us be a success in the land of medical care giants. All hospitals are trying to do a good job. All hospitals are asking what is the right technology to do the best thing for our patients.”
“I do not see these technologies as economic lifesavers. I don’t think that works,” he said. “When all is said and done, it’s going to be whether people believe York Hospital is doing the right thing for their well-being.”
–
As of November 2017, Portsmouth Regional Hospital has obtained the GPS technology a allowing patients access to the same benefits in Portsmouth.
To view the article on Seacoast Online, visit http://www.fosters.com/news/20170828/york-hospital-using-new-shoulder-replacement-technology.